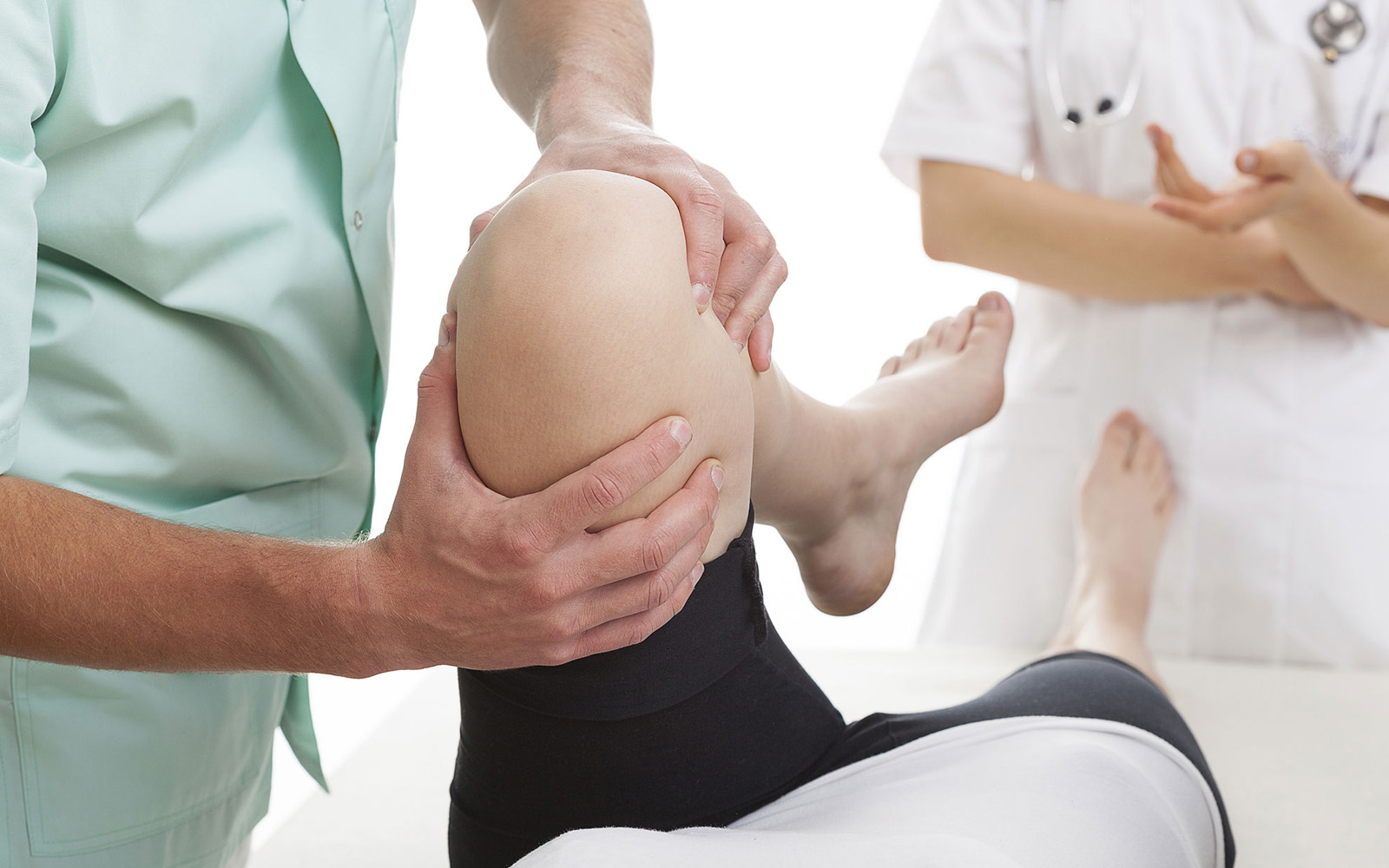
Knee pathology can be accurately diagnosed with a thorough patient history and physical examination. Physical examination by an orthopaedic surgeon or trained musculoskeletal specialist, along with an understanding of knee anatomy and biomechanics, can be used to reliably diagnose most meniscal and ligamentous injuries. Radiography should be performed for all patients with knee injury, and weight-bearing views should be obtained when arthritis is suspected. MRI, which can be helpful in some cases, is not always necessary and should never be performed in lieu of a history and physical examination.
After a good history is taken, the location of pain and any mechanical symptoms should be identified, along with the mechanism of injury. Previous injuries should be described because the current injury may be the sequela of a prior incident. Knee examination includes active and passive range of motion (ROM), palpation, and special tests, with any potentially uncomfortable tests performed last.
To ensure a thorough examination, both of the patient’s lower extremities should be fully exposed. An assessment of gait should be performed first, looking for varus or valgus, quadriceps avoidance, and antalgic gaits. Substantial primary varus or valgus deformity may be the result of single-compartment osteoarthritis. With quadriceps avoidance, the patient bears weight with a knee locked in extension because of either a weakened extensor mechanism or pain. An antalgic gait can result from any condition causing knee pain.
Next, an assessment of standing limb alignment should be performed, taking note of specifics, such as pes planus and excessive femoral anteversion, both of which can contribute to patellofemoral tracking problems. Excessive femoral anteversion may be identified by an inward-pointing or so-called squinting patella. The musculature, particularly the quadriceps, should be inspected for atrophy. In addition, the patella should be assessed for malalignment, which may predispose the patient to maltracking or patellar dislocation. Patella alta or baja is generally assessed with the patient in the seated position and can be confirmed radiographically.
Any localized swelling and masses, including swelling of the prepatellar bursa, a meniscal cyst, and Osgood-Schlatter disease of the tibial tubercle, should be noted. A popliteal (ie, Baker) cyst can be palpated posteriorly with the knee extended. Swelling of the distal femur or proximal tibia may indicate a neoplasm or infection.
The knee should be inspected for a prepatellar or intra-articular effusion. An effusion of the prepatellar bursa is anterior to the patella; with an intra-articular effusion, the patella remains palpable subcutaneously. On inspection, a true knee joint effusion is often best appreciated in the suprapatellar pouch.
Compared with the contralateral knee, the injured knee may fail to reach full passive extension, which may indicate a mechanical block or hamstring spasm. Limited ROM is expected with large knee effusions or pain. Although full ROM is required for a complete knee examination, it is not always possible at the first visit and should not be forced.
Palpation should be done systematically, altering the approach depending on the area of discomfort and examining the area of reported pain last. Palpation of all structures including the patella facets, the collateral ligaments, the menisci, the patella tendon, the tibial tubercle and the popliteal fossa is important. Finally, it is important to remember that pain felt in the knee may be referred from other locations, including the spine and the hip. A careful history can help differentiate referred spinal or hip pain. Routine examination of the hip and spine is recommended when evaluating knee pain, with particular attention paid to loss of hip rotation.
Reference:
Physical Examination of the Knee: Meniscus, Cartilage, and Patellofemoral Conditions. Bronstein, Robert D. MD; Schaffer, Joseph C. MD
JAAOS - Journal of the American Academy of Orthopaedic Surgeons: May 2017 - Volume 25 - Issue 5 - p 365–374
doi: 10.5435/JAAOS-D-15-00464