Psoriatic arthritis (PsA) is a chronic autoimmune disease that causes inflammation of the skin and joints. Skin can become itchy and scaly, and the inflamed joint areas can become stiff, swollen, and painful. It is estimated that as many as 30% of people who have psoriasis will also develop Psoriatic arthritis. However, as it is sometimes activated in the joint area before symptoms appear on the skin’s surface, people can mistake it for osteoarthritis (OA) since both forms of arthritis display shared symptoms of joint pain, swelling, stiffness, and reduced flexibility. In this article, we will be looking at psoriatic arthritis vs osteoarthritis radiology, causes and symptoms, and other facts you should know about the two forms of arthritis.
What’s the difference Between OA and PsA?
The difference is that osteoarthritis is not an autoimmune disease like PsA but is a form of degenerative joint disease promoted by the wear and tear of cartilage and bones rubbing together. Similar to psoriatic arthritis, OA exhibits the inflammation and pain symptoms mentioned above, and in serious cases or without proper self-management, it can immobilize people.
Psoriatic arthritis (PsA) and osteoarthritis (OA) are the two most common forms of arthritis. Osteoarthritis is a consistent condition, whereas PsA can flare up irregularly. Other unique symptoms associated with OA include grinding and clicking of the joint area during movement, distorted joint shape, and hard lumps of bone growth near the joint. Symptoms specific to PsA include a red rash and silvery-white patches on the skin, nail pitting, swollen fingers and toes, eye redness and pain, tendon and ligament pain, and fatigue.
Is Psoriatic Arthritis Worse than Osteoarthritis?
The progress of your PsA or OA determines the severity and whether one or the other is worse. Some cases of PsA are mild, and since flares can come and go, it may not interfere with a person’s life as much as the constant OA can. Severe cases of osteoarthritis can create daily discomfort and pain. Both require proper self-management to mitigate pain and slow the progression of the diseases. If conditions are misdiagnosed or treated inappropriately, it can have a debilitating effect on the person suffering from arthritis.
Can you have Psoriatic Arthritis and Osteoarthritis at the Same Time?
The risk for OA in patients with PsA is significantly higher than for those who do not suffer from the condition, with the prevalence of OA being 22.1% in the PsA group. This overlap can prove difficult when identifying and x-raying psoriatic arthritis and osteoarthritis. An incorrect diagnosis can lead to the wrong treatment of medication and therapy, and as a consequence, the condition worsens. Looking out for symptoms unique to each condition, in addition to radiology procedures, go hand in hand to ensure an accurate diagnosis.
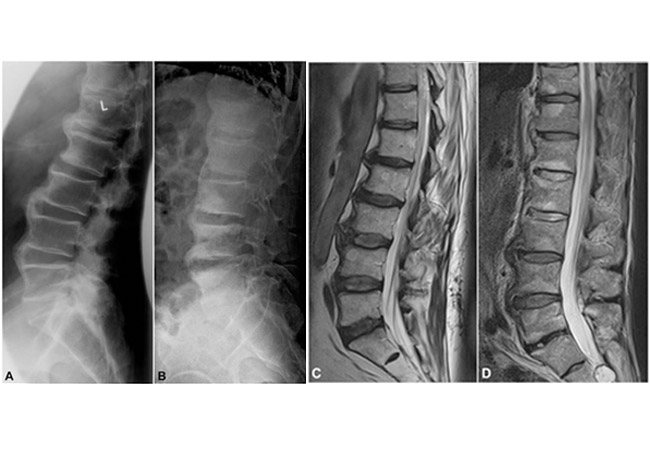
5 Facts You Should know about Psoriatic Arthritis vs Osteoarthritis
To summarize the causes and symptoms of both Psoriatic Arthritis and Osteoarthritis, here are five important facts to know.
1. PsA Causes
Psoriatic Arthritis doesn’t have one clear determiner which triggers the disease; however, the following risk factors can promote PsA;
- • Psoriasis: more than eight million people have psoriasis in the U.S.
- • Immune abnormalities, i.e., higher levels of certain proteins in the blood such as cytokines, which trigger inflammation.
- • Environmental factors: such as a bacterial or viral infection and physical trauma.
- • Genetics: approximately 40% of people with psoriasis or psoriatic arthritis have family members with psoriasis or psoriatic arthritis.
2. OA Causes
Osteoarthritis is a result of the wear and tear when the cartilage that supports the bones in your joints progressively deteriorates. The following factors can increase the risk of OA;
- • Genetics and Gender: Studies have shown that the influence of genetic factors is between 39% and 65% in radiographic OA of the hand and knee in women, around 60% in OA of the hip, and approximately 70% in OA of the spine. Women are also more likely to get OA.
- • Obesity: Weight adds pressure to your joints, which ultimately wears the cartilage down and once the bone is painfully rubbing against bone, it can become a severe problem.
- • Joint Injury or malformation: if joints have been damaged or haven’t formed normally, there is an increased chance of having OA.
- • Age: the chance of getting OA increases as you get older, particularly over the age of 50.
3. PsA Symptoms and Treatments
Symptoms of PsA can include the following;
- • A red rash and/or silvery-white patches on the skin
- • Nail pitting
- • Swollen fingers and toes
- • Eye redness and pain
- • Tendon and ligament pain
- • Fatigue
Some of the common treatments of PsA include;
- • Topical treatments for skin and nail irritations
- • Medication and steroid injections to reduce inflammation and pain
- • Joint replacement surgery for severe cases
4. OA Symptoms and Treatments
Symptoms of OA can include the following;
- • Grinding and clicking of the joint area when moving
- • Pain and stiffness of joints affected
- • Inflammation
- • Decreased flexibility and immobility
Some of the treatments available to those with OA to reduce inflammation, relieve pain, improve mobility, and slow progression include;
- • An exercise plan to lose weight to decrease pressure on joints
- • A modified diet to reduce intake of inflammation-inducing foods and to maintain a healthy weight
- • Medication and supplements
- • Therapies such as acupuncture and exercises to strengthen areas with OA
- • Invasive treatments such as a joint replacement for severe cases or cortisone injections.
5. Management of PsA and OA
As each person experiences individual symptoms, the many different options available in terms of treatment and management of psoriatic arthritis and osteoarthritis may not be suitable for your specific needs. It is always best to get advice from professionals and learn how to self-manage your arthritis with support from personalized programs and communities dealing with the same condition. Keeping connected with your loved ones is important, as arthritis can take a toll on your mental wellbeing.

Final Thoughts
With two of the most common forms of arthritis having the potential to overlap, you must ensure that whether you are currently experiencing psoriatic arthritis or osteoarthritis, you have a clear diagnosis and treat each condition individually to alleviate the symptoms of both and to maintain mobility. If you are experiencing any of the shared symptoms of joint pain, swelling, stiffness, and reduced flexibility but do not show any signs on the skin, it is best to consult with a doctor for a clinical diagnosis. When you understand the underlying condition, you can proactively self-manage and live a normal life.





